Disorders of Consciousness Program
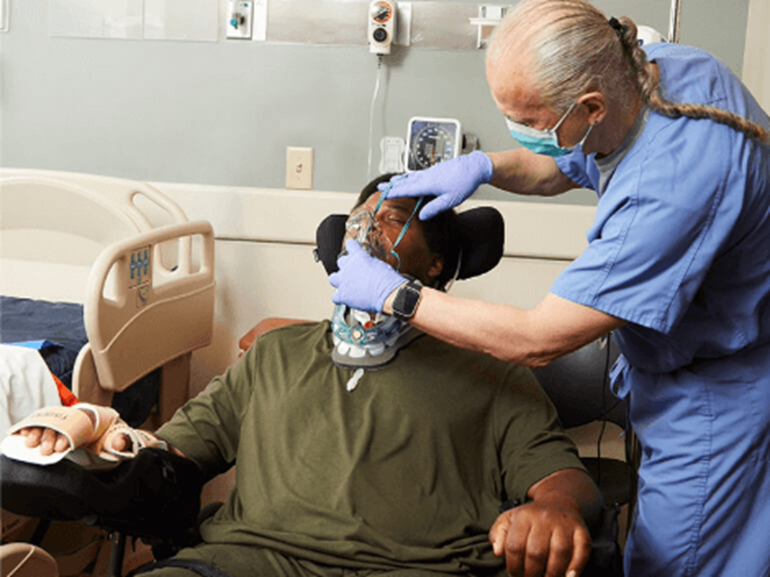
About the program
Our top priority is to help you bring your loved one home. We address responsiveness and identify a means of communication for family members as best as possible.
The Disorders of Consciousness (DoC) Program at Baylor Scott & White Institute for Rehabilitation – Dallas provides specialized assessment and treatment for improving function in individuals with a disorder of consciousness. Detailed education and training for caregivers plays a big part in this program and is critical to being able to bring your loved one home.
Our DoC program meets and exceeds all requirements for treating persons with disorders of consciousness set forth by the American Congress of Rehabilitation Medicine and the Traumatic Brain Injury Model Systems (TBIMS) program, sponsored by the National Institute on Disability, Independent Living, and Rehabilitation Research (NIDILRR).
We draw on the knowledge of an experienced team of brain injury specialists to address the range of medical, physical, functional and emotional issues you face. This interdisciplinary team is led by a physiatrist, a physician board-certified in physical medicine and rehabilitation, and includes rehabilitation nurses; physical, occupational, speech, respiratory and recreation therapists; psychologists and neuropsychologists; dietitians; case managers; and other clinical and support staff as needed.
Together, we optimize the recovery of individuals at every level of injury from those in a minimally conscious state to those with mild traumatic brain injury.
Eligible patients
Patients appropriate for this program are no longer in a coma (meaning their eyes are open at least some of the time), but have not regained a level of consciousness that allows them to respond consistently to their environment, communicate reliably or complete basic self-care activities.
- Age 15-64 years
- Traumatic Brain Injury less than one year post onset
- Non-traumatic brain injury (can include Anoxia, CVA, Metabolic encephalopathy) less than three months post-onset
- Medically stable
- Established discharge plan home with family/caregivers providing 24/7 care
Exclusion criteria:
- Ventilator dependent
- No/limited support to discharge home
Program details:
- Requires extensive preadmission workup with a 30-minute family meeting in person or on the phone with Dr. Dubiel and/or TBI Coordinator
- Requires discharge disposition established and benefit verified
- Family presence and participation is required as follows:
- Week 1: 2-3 days of treatment
- Week 2: 3-4 days of treatment, two nights
- Week 3: all day treatment
- Team to include: MD, CM, NP, PT, OT, ST
- 180 minutes of therapy per day Monday through Friday, including four 45-minute sessions of any combination of PT, OT, ST, NP; includes weekend therapy; will receive 15 hours of therapy over seven days a week (automatic medical order written)
- Employ services of: neurosurgery, neurology, EEG, ITB pump trials, palliative care as applicable
- Admit on Tuesday, Wednesday, Thursday ONLY
Frequently asked questions
-
The Disorders of Consciousness program at BSWIR Dallas has a standardized 21 day program.
-
The goals of the three week program include addressing responsiveness and, as best as, possible identify a means of communication for your loved one. Additionally, our goal is to train you to care for and advocate on the behalf of your loved one. We will also identify and order equipment to prepare your loved one to discharge from the hospital setting.
-
While we are hopeful your loved one will emerge from the disorders of consciousness state and move into our active TBI program, we do anticipate your loved one needing full time care.
-
The goal of the program is to equip families with education, training and equipment for caring for their loved one in a home environment and is designed for families committing to bringing their loved one home upon completion. Home Health services, such as therapy and nursing, will likely be recommended, as well as options for hired caregivers as desired. Securing alternate discharge plans, such as skilled nursing facilities, nursing homes and assisted living facilities can be challenging due to barriers such as age, presence of tracheostomy, insurance approval, diagnosis and medical complexity.
A leader in Traumatic Brain Injury Research
Baylor Scott & White Institute for Rehabilitation is one of only 16 organizations in the nation designated as Model System of care. The North Texas Traumatic Brain Injury Model System has been funded since 2002 and provides the largest continuum of care to individuals with TBI in North Texas and surrounding states. This continuum includes emergency medical services, acute care, rehabilitation and outpatient services. Learn more about the TBI Model System.
Let us help.
Our top priority is to help bring your loved one home.